It’s one of the most common symptoms of menopause and fluctuating hormones, yet one that faces significant stigma. Any guesses?
You got it, we’re talking about vaginal dryness.
Vaginal dryness develops in a majority of women who undergo the menopause transition. And, for some women, vaginal dryness can occur as a medication side effect or from breastfeeding. Yet many women hesitate to discuss vaginal dryness with their providers or are unaware effective treatments exist.
We must normalize symptoms like vaginal dryness so that more women can understand why it happens, what it feels like, and what they can do to find relief. With that in mind, here are the top three things women need to know about vaginal dryness.
What is vaginal dryness?
As many as 50% of women experience vaginal dryness during and after the menopause transition. When a woman enters perimenopause, their estrogen levels begin to decrease. Estrogen, a primary reproductive hormone, helps produce vaginal discharge that keeps the vulva and vaginal lining elastic and lubricated, and lactobacilli, a bacterial strain that protects the vagina from infection. Without enough estrogen, the vagina produces less and less discharge and protective bacteria, contributing to a dry and infection-prone environment.
Blood flow to the vagina also decreases as estrogen declines and, as a result, the skin around the vagina thins. Some refer to this combination of estrogen-related symptoms as vaginal atrophy. Though most women who experience vaginal atrophy are also undergoing menopause or are postmenopause, vaginal dryness can occur at any age.
Other causes of vaginal dryness are typically either hormone or non-hormone related. Certain medications for cancer treatments, autoimmune conditions, smoking, severe stress, and breastfeeding can cause estrogen levels to drop and vaginal dryness to develop.
Other types of medications, including those for allergies and colds, may not interfere with your estrogen levels but can still contribute to vaginal dryness symptoms. If you suspect none of these factors contributes to your vaginal dryness, you may want to check for irritating ingredients in your body wash or detergent and speak with a healthcare provider.
What does vaginal dryness feel like?
Vaginal dryness can appear as a host of different symptoms. Many women first notice vaginal dryness when they experience pain during sex, also called dyspareunia. However, vaginal dryness symptoms can develop over time. For some women, this may mean milder symptoms during perimenopause and more intense symptoms postmenopause.
Women with vaginal dryness also vary in symptom severity and sensitivity. For example, some report only itchiness, while others may experience soreness or irritation. It’s also common to develop urinary frequency or urinary tract infections (UTIs) and yeast infections alongside vaginal dryness from a lack of estrogen-producing lactobacilli.
How do you relieve vaginal dryness?
Vaginal dryness may not upend your day-to-day routines, but it can cause significant discomfort. Discomfort women do not need to endure. Because vaginal dryness can carry a certain stigma, women are often unaware help exists.
For mild and moderate vaginal dryness, the first line of evidence-based options are vaginal moisturizers and personal lubricants. Vaginal moisturizers add hydration to the lining of your vagina and can help strengthen your vaginal tissue. Personal lubricants reduce pain during sex and can be used in addition to a vaginal moisturizer.

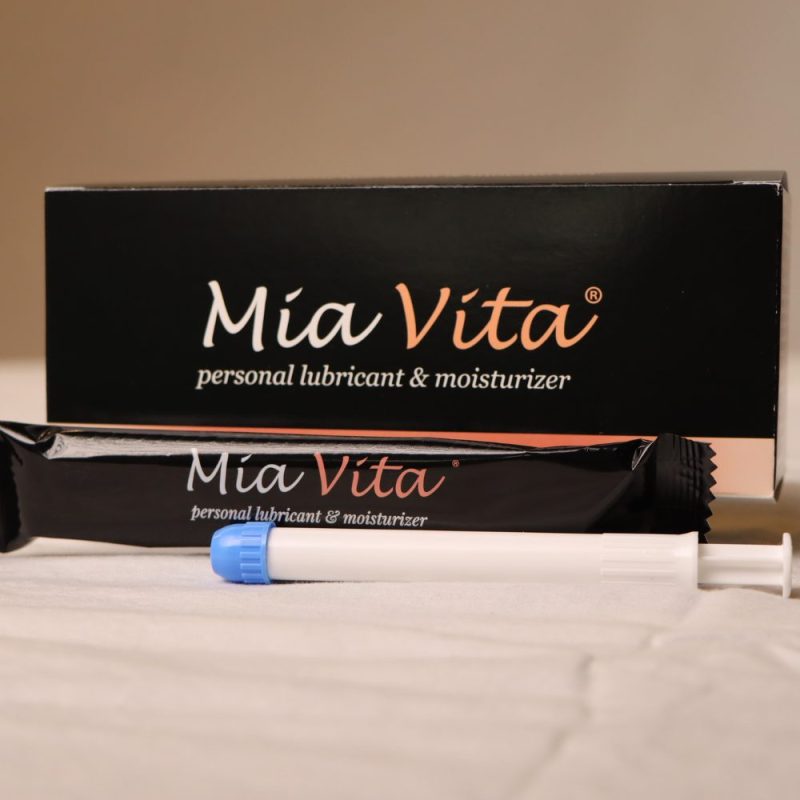
The Mia Vita Personal Lubricant and Vaginal Moisturizer addresses these needs in one effective product that helps relieve itching and irritation and increases comfort during sex. With an easy-to-use, mess-free applicator, the product is also FDA-cleared as effective for internal vaginal use.
Ingredients in the Mia Vita Personal Lubricant and Moisturizer, like sodium hyaluronate and Vitamin E, help your vagina retain more moisture and a sufficient water balance over time. Studies also show water-based moisturizers and lubricants are reported to have fewer side effects than other primary ingredients. For maximum benefit, most women use the product every day for 20-28 days, then every couple of days to maintain its benefits and find long-term relief.
Some women with more severe vaginal dryness symptoms may benefit from hormone replacement therapy (HRT) to relieve vaginal dryness, either in the form of low-dose estrogen creams or higher doses in pills or patches. However, when it comes to HRT, it’s best to talk with your provider to determine the best option for you.
Certain lifestyle choices can also help reduce your risk for or the severity of vaginal dryness. Regular sex, with lubrication, can increase blood flow to your vagina and strengthen your vaginal tissue. Try not to wash inside your vagina, and avoid using harsh soaps on your vulva.
FemmePharma has been helping women navigate menopause for over two decades. No matter where you are in your journey, you deserve to have knowledgeable, intimate healthcare partners to help you feel your best. Explore our other articles, podcast episodes with women’s health experts, and products to ease your transition into menopause.