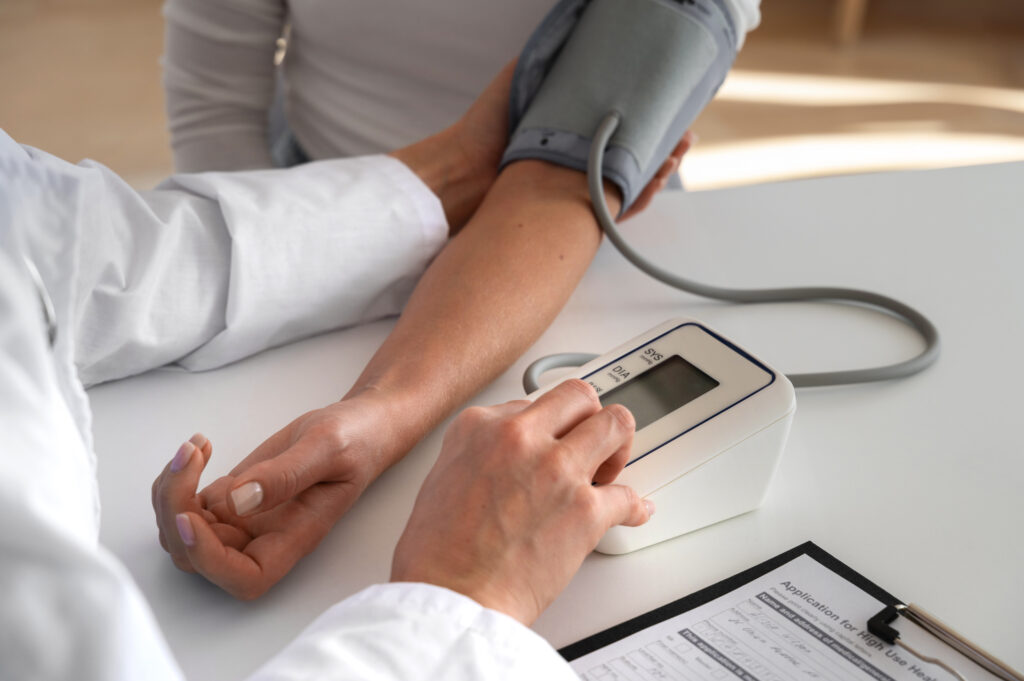
Perimenopause and postmenopause can mask symptoms of high blood pressure. However, for women undergoing the menopause transition, the risk for high blood pressure increases. Why does this happen, and what can you do to manage and lower your blood pressure during menopause?
Hormonal changes and blood pressure: how menopause impacts women’s heart health
People often think of heart conditions as affecting more men. For instance, in commercials and other media alerting the public to watch for signs of a heart attack, it’s often a man clutching his chest.
But the numbers tell a different story.
Women account for 52% of deaths from high blood pressure, and according to the CDC, about 44% of women in the US live with heart disease. Age accounts for some of this percentage, as blood pressure does rise with age, but not all.
Hormonal changes, stress, genetics, and even weight gain all amount to significant high blood pressure risk factors. Women who experience high blood pressure during pregnancy and women who undergo early menopause are also at greater risk for rising blood pressure during the menopause transition.
What’s the connection between menopause and high blood pressure?
Before undergoing the menopause transition, women report lower blood pressure levels than men, but that flips for postmenopausal women. Why is this the case? Researchers found that estrogen protects the arteries. Estrogen has what’s referred to as a “vasodilative effect,” which means it keeps blood vessels flexible and open enough for blood to flow freely. When estrogen levels start to drop during perimenopause, your arteries can begin to stiffen and slow blood flow.
Less estrogen can also contribute to increased plaque production, a buildup of fat and cholesterol, which can stick to and narrow artery walls. Restricted blood flow increases the pressure on artery walls and, over time, can lead to a diagnosis of high blood pressure. If left untreated, high blood pressure can cause permanent artery damage and long-term heart problems.
But most often, there are little to no physical symptoms of high blood pressure. Moderate signs and symptoms of high blood pressure, like chest pain, headaches, and fatigue, are often attributed to menopause-related symptoms in middle-aged and older women. Or, when women do raise heart-related concerns, they are often thought to be “stress” or “hormone-related issues.” So, when a woman is finally diagnosed, it’s often with moderate or more severe high blood pressure levels.
How to prevent high blood pressure throughout menopause
One of the biggest takeaways from learning about the connection between high blood pressure and the menopause transition? The need for greater awareness. Up to 50% of women will develop high blood pressure before they turn 60. The more women are aware of their risk for high blood pressure, the sooner they can take action to mitigate their risk factors, make preventative healthcare appointments, and share this information with friends and family.
Researchers also agree that high blood pressure risk factor identification needs improvement among menopausal women, as does research about its origins. For example, there’s little research about how and when women’s blood pressure changes perimenopause, only that it does as estrogen declines.
Hormone replacement therapy (HRT) and its impact on blood pressure
Some providers prescribe hormone replacement therapy (HRT) to women with low-risk profiles to ease menopausal symptoms. Some women who start taking HRT earlier may benefit from certain “cardiovascular benefits,” but not those who start HRT later on during the menopause transition.
However, recent research found some women who take estrogen-only HRT may be more likely to develop high blood pressure than women who take other forms of HRT. These reports do not mean all HRT causes high blood pressure; instead, this particular kind (estrogen only) may increase a woman’s chances of developing high blood pressure. The delivery method of HRT may also play a role, as one study noted that oral estrogen-only HRT may also contribute to higher blood pressure levels versus other methods.
How to lower blood pressure during the menopause transition
Prevention remains critical to preventing heart problems like high blood pressure in menopausal women. The best way to prevent rising blood pressure is to make regular appointments with your healthcare provider. Your provider can measure and track any changes to your blood pressure and recommend fitting treatments and preventative methods as needed.
Maintaining a healthy heart during perimenopause and postmenopause often comes down to lifestyle. According to the American Heart Association, everyone should aim for two and a half hours of physical exercise a week. Eating a heart-healthy diet full of vegetables and other fibrous foods can also benefit your heart, as can getting plenty of sleep each night. Heart health experts also recommend avoiding high-sugar and processed foods that can contribute to clogged arteries.
Changing your lifestyle habits can seem daunting, but focusing on one change at a time and taking small steps can lead to a profound transformation in your heart health as you navigate the menopause transition.
FemmePharma has been helping women navigate menopause for over two decades. No matter where you are in your journey, you deserve to have knowledgeable, intimate healthcare partners to help you feel your best. Explore our other articles, podcast episodes with women’s health experts, and products to ease your transition into menopause.