Yearly mammograms are a necessity for women beginning at age 45, and sometimes sooner for those with risk factors like a family history of breast cancer. Mammography has helped reduce the breast cancer mortality rate by 40 percent since 1990. But if you’ve never had a mammogram, you probably have a lot of questions. And we have answers.
What is a mammogram?
According to cancer.org, a mammogram is a low-dose X-ray that allows your doctor to look for changes or abnormalities in breast tissue, often well before you notice a lump. There are two types: screening and diagnostic.
A screening mammogram looks for signs of breast cancer in women with no known symptoms. During the procedure, your doctor takes two X-rays of each breast at different angles.
A diagnostic mammogram further examines abnormalities found during a screening. During this procedure, doctors take additional images of each breast and compare them to the screening results. Doctors also perform diagnostic mammograms on women who have symptoms of breast cancer.
What happens during the test?
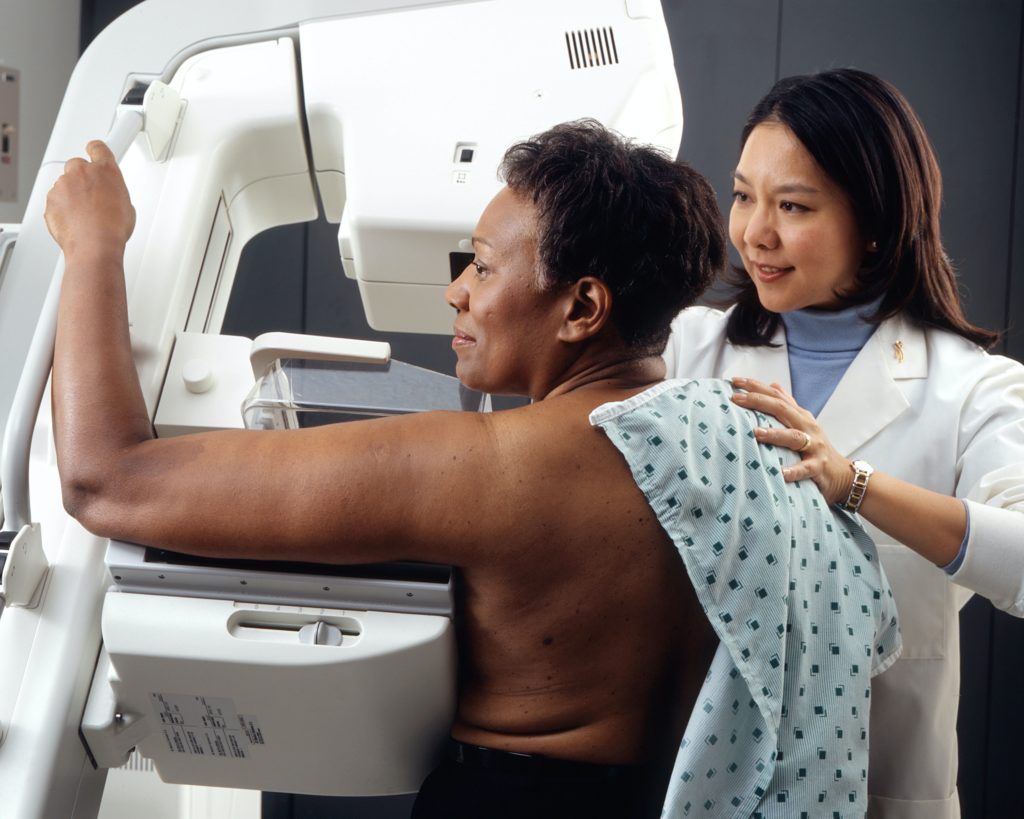
During a mammogram, your doctor will use a machine designed to only look at breast tissue. Since it’s difficult to process X-rays through breast tissue, the machine contains two plates to compress the breast to allow for more accurate images with less radiation. You’ll be asked to place one breast at a time on the bottom plate. Your doctor will lower the top plate to flatten your breast and take the X-ray. Digital mammograms are common these days; the technician records the images and saves them to a computer. Three-dimensional mammograms allow for a more precise view of breast tissue. Your health insurance may not cover a 3D mammogram, and in some cases, these require more exposure to radiation.
Does a mammogram hurt?
Since the machine compresses your breast during the mammogram, it is possible that you’ll feel some discomfort. The good news is that it lasts only for a few seconds, and it shouldn’t take more than 15 minutes to do your full mammogram. When you weigh that against the consequences of not having a mammogram — like a battle with breast cancer — it seems like a fair trade-off.
Are mammograms safe?
There’s a common misconception that mammograms expose the body to unsafe levels of radiation, but this isn’t true. According to hopkinsmedicine.org, mammograms use only a small amount of radiation, and it is within medical guidelines. We are exposed to various levels of background radiation daily. The amount of radiation from a mammogram is equal to about two months of exposure to background radiation. But don’t worry! Mammography is regulated by the U.S. Food & Drug Administration.
Are they accurate?
Yes. According to komen.org, mammography correctly identifies 87 percent of women who have breast cancer. Women over the age of 50 have a higher sensitivity to mammograms, meaning that their accuracy can be even greater.
False positives do happen. However, the chance of having one after having one mammogram ranges 7 percent to 12 percent. They are more common among young women and women with dense breast tissue. Additionally, the more mammograms you get, the more likely you are to experience a false positive. It’s unfortunate, but that’s why it’s important not to panic if your doctor calls you back after an abnormal mammogram.
How to prepare for a mammogram
- Avoid scheduling the mammogram a week before your period if possible, since this is when your breasts are most sensitive.
- Take a list of past biopsies or other breast treatments if you’ve had any. This list can help prevent false positives.
- On the day of your exam, don’t wear antiperspirant or deodorant, since some of the substances in them can show up as white spots. Instead, take deodorant with you so you can apply it after your exam.
- Tell your doctor about any changes in your breasts ahead of time.
What happens afterward
You will likely get a letter in the mail that gives you the all clear. You could also get a letter or a phone call that asks you to come in for more pictures. If that happens it can be hard not to be stricken with worry, but try not to stress. Since doctors don’t have a baseline to which they can compare the results, women who have just had their first mammogram commonly require a follow-up. It’s also common for those who are pre-menopause. Fortunately, fewer than one in 10 women who get called back have cancer.
Schedule a mammogram
If you’re 45 or older and have never had a mammogram or younger than 45 and have a family history of cancer or other breast concerns, speak with your doctor. When it comes to breast cancer, early detection can be a matter of life and death.
If you’re perimenopausal or post-menopause, breast cancer prevention isn’t the only thing on your mind. You may be experiencing vaginal dryness, hot flashes, sleeplessness, and more. And we’re here to help.